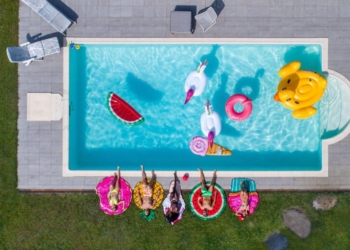In late February 2024, Change Healthcare, a subsidiary of UnitedHealth Group, fell victim to a cyberattack that has since sent ripples across the healthcare sector. The incident not only compromised the company’s operations but also had a profound effect on Medicaid payments, leaving providers and beneficiaries in a state of uncertainty.
The cyberattack on Change Healthcare was more than just a breach of security; it was an assault on the lifeline of healthcare providers who rely on timely Medicaid reimbursements. In the wake of the attack, providers found themselves unable to submit claims, leading to a significant cash flow crunch. The disruption was felt most acutely by smaller practices, which operate on thinner margins and depend heavily on consistent payment cycles.

CMS’s Swift Response
In the immediate aftermath of the cyberattack, CMS took decisive action to mitigate the impact on healthcare providers and ensure continuity of care for patients. They announced a series of measures aimed at providing financial relief and operational support to those affected.
CMS recognized the urgent need for financial support and responded by considering applications for accelerated payments for Medicare Part A providers and advance payments for Part B suppliers. This swift financial assistance was crucial in maintaining healthcare services and alleviating the cash flow challenges faced by providers.
To further ease the burden, CMS introduced operational flexibilities, including expedited claims processing and guidance for Medicare Advantage and Part D programs to relax prior authorization and filing requirements. These measures were essential in helping providers navigate the challenges posed by the cyberattack.
CMS also worked closely with state agencies, urging Medicaid managed care plans to make prospective payments to impacted providers. This collaborative effort ensured that Medicaid beneficiaries continued to receive uninterrupted access to services.
The Road to Recovery
As Change Healthcare worked towards restoring its services, the focus shifted to recovery and building resilience against future cyber threats.
Change Healthcare implemented a phased reconnection process for its key products, prioritizing the restoration of services critical to the healthcare system’s operation. This included eligibility processing, claims pricing, and pharmacy electronic claims, among others.
The cyberattack highlighted the need for robust cybersecurity measures. In response, Change Healthcare, along with UnitedHealth Group, took significant steps to enhance their security protocols and infrastructure to prevent similar incidents in the future.
The incident served as a wake-up call for the healthcare industry, emphasizing the importance of cybersecurity preparedness. It sparked a broader discussion on the need for industry-wide collaboration and investment in security measures to protect sensitive health information.